Benefits of Quality Stethoscopes
High-quality medical stethoscopes are crucial for effective patient care, offering several key advantages:
- Accurate Diagnoses: Enhanced sound clarity allows for precise assessments. For instance, detecting a subtle heart murmur early can lead to more effective treatment options for patients, significantly impacting recovery outcomes.
- Durability: Built to withstand the rigors of daily use, these stethoscopes reduce the need for replacements, ensuring reliability when it's needed most. Consider a scenario where a doctor can always rely on their instrument during critical examinations, enhancing the continuity of care.
- Comfort: Ergonomically designed for extended wear, they prevent discomfort for healthcare professionals during long shifts. This aspect is vital for maintaining focus and efficiency, especially during back-to-back patient consultations.
Our stethoscopes come equipped with cutting-edge features like advanced acoustic sensitivity for detecting low-frequency sounds, noise-cancellation technology to eliminate ambient interference, and ergonomic designs for better handling and comfort. These innovations support superior performance and ease of use.
Choosing the Right Stethoscope
Selecting the appropriate stethoscope requires careful consideration of several factors tailored to the user’s professional demands and personal preferences. These include the practitioner’s specialty, how often the stethoscope will be used, and budgetary constraints. Important features to evaluate are the chest piece material, which affects sound transmission and durability; the tube length, impacting ease of use and comfort; and the diaphragm type, determining the range and quality of sounds captured. Understanding these elements ensures the stethoscope aligns with your specific clinical needs, enhancing diagnostic accuracy and patient care efficiency.
Product Range and Descriptions
Our stethoscope lineup includes:
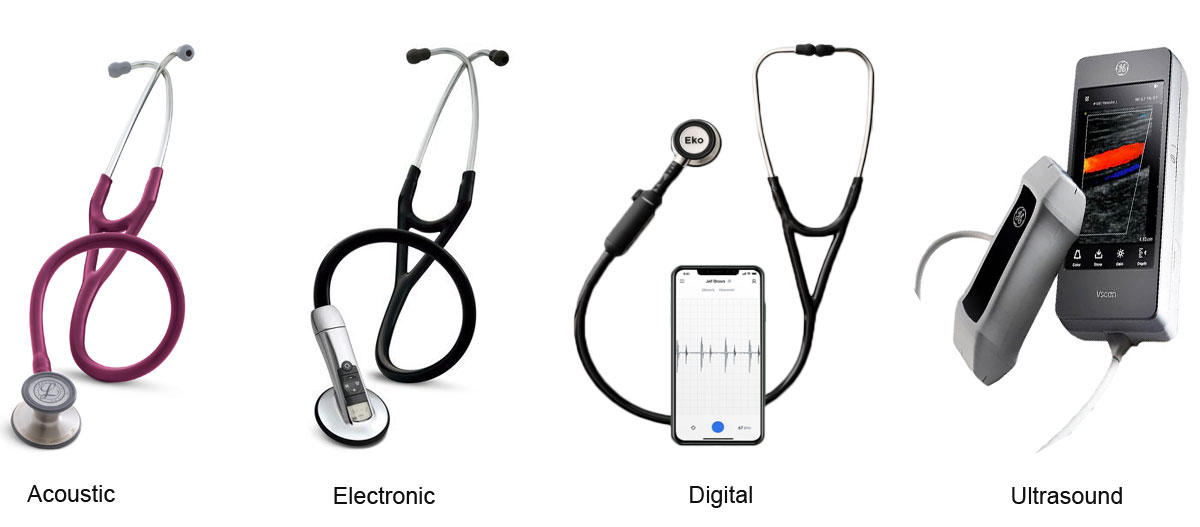
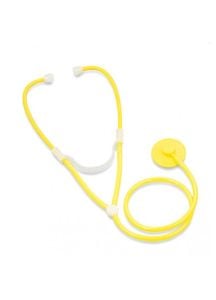
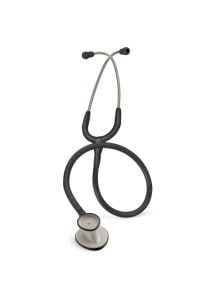
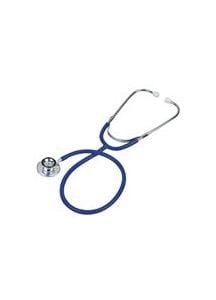
- Acoustic Stethoscopes: Ideal for general use, providing clear acoustic performance.
- Electronic Stethoscopes: Amplify sounds for detailed hearing.
- Pediatric Stethoscopes: Specially sized for young patients.
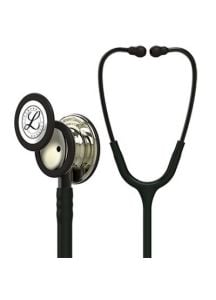
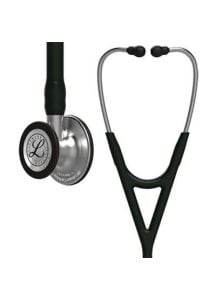
- Cardiology Stethoscopes: Offer enhanced sensitivity for cardiac assessments.
- Ultrasound Stethoscopes: Advanced imaging for precise diagnostics.
FAQs (Frequently Asked Questions)
Q: How do I choose the right stethoscope for my needs?
A: Consider your specialty and the type of patients you see. Acoustic stethoscopes are great for general use, while electronic models can amplify sound for detailed diagnostics. Pediatric stethoscopes are designed for children, and cardiology stethoscopes offer enhanced sensitivity for heart assessments. Also, think about the chest piece material, tube length, and diaphragm type to ensure the stethoscope meets your specific requirements.
Q: Can I use the same stethoscope for adults and children?
A: While some stethoscopes are versatile, we recommend using a pediatric stethoscope for children to ensure comfort and accuracy. Pediatric stethoscopes have smaller chest pieces and diaphragms tailored for young patients.
Q: How do I maintain and clean my stethoscope?
A: Regular cleaning is essential for hygiene and performance. Use a mild soap and water solution or alcohol wipes to clean the ear tips, diaphragm, and tubing. Avoid submerging your stethoscope in liquid or exposing it to extreme heat or cold.
Q: Are there any special care instructions for electronic stethoscopes?
A: Electronic stethoscopes should be kept away from moisture and extreme temperatures. It's also important to check the batteries regularly and replace them as needed to ensure optimal performance.
The Top Brands
Highlighted here are leading brands available, distinguished by their superior quality, dependability, and innovative contributions to medical diagnostics.
- Littmann
- MDF Instruments
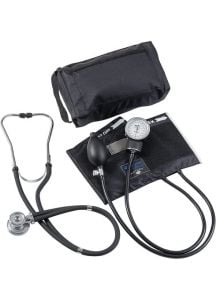
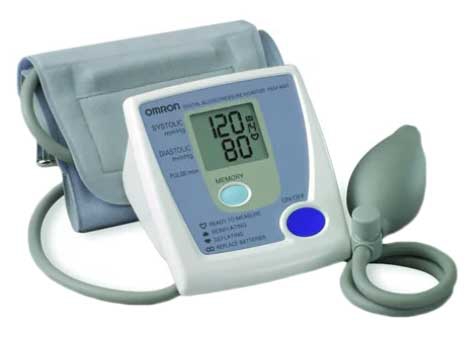
- Omron
- American Diagnostic ADC

Product Videos






















Login and Registration Form