Blood saturation meters detect hypoxemia or low blood-oxygen levels at the extremities from the heart, including the hands and feet. Measurements at these extreme locations provide a more accurate picture of how efficiently blood is transporting oxygen throughout the body. An oxygen reading between 95 and 97% is normal, according to the American Lung Association. Any reading below 95% would justify a call to a doctor. A reading below 90% would be a reason to visit the emergency room.1 Heart rate oximetry monitoring significantly reduces perioperative hypoxemia. It enables the detection and treatment of hypoxemia and related respiratory maladies.2 Heart rate monitors are not expensive, making them ideal for home diagnostics. They are compact and easy to use.
Profile of O2 Sensor Readers
Product Advantages
- Adaptability to Home Care Use
- Applicable to a Wide Range of Clinical Settings
- Ease of Use
- Portability
- Illness Detection
Using an O2SAT device can detect low-oxygenation in a patient before it reaches a dangerous level. The use of blood oxygen detectors is mostly on a conscious patient, but their use in surgery is a common practice, particularly when a patient is under anesthesia. O2 monitors are also used for sleep studies, prevention of sudden infant death syndrome (SIDS), exercise sports training, and often when a patient is receiving adjunct oxygen therapy.
Sleep studies use O2 sensors to monitor a patient's tendency to stop breathing during sleep. When an individual stops breathing during sleep, this is termed 'sleep apnea.' Regular periods of sleep apnea creates low oxygen levels in the blood and interferes with the regular sleep cycle. These patients often complain of a lack of feeling well-rested. Some blood oxygen monitors have software that allows recording the trend of oxygen saturation during a sleep cycle. O2 sensors used for people who have sleep apnea come with an alarm that sounds when the saturation reaches a pre-set threshold.
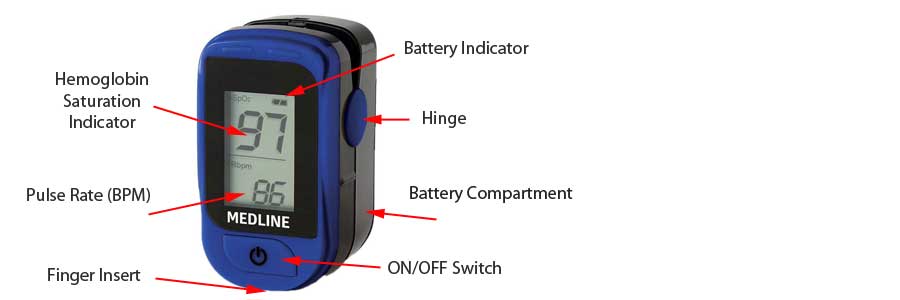
Anatomy of a Pulse Ox Monitor
Below is a list of conditions that a patient may have that may require monitoring their blood oxygen level.
- Anemia
- Asthma
- Chronic obstructive pulmonary disease (COPD)
- Congenital heart defects
- Heart attack
- Heart failure
- Lung cancer
- Pneumonia
Common Assessments with O2 Sensors
- assesses how well a new lung medication is working
- determines patient-ventilator effectiveness
- evaluates whether someone needs help breathing
- examines the effectiveness of supplemental oxygen therapy
- tests the efficacy of sleep apnea therapy
- observes oxygenation during a sleep study
- monitors oxygen levels during surgical procedures
- detects post-surgical patient oxygenation
- assesses oxygen levels during physical activity
Many recent purchases of SpO2 devices are a result of COVID-19. Consumers purchase the devices to home-detect low oxygen saturation levels—one of the signs of COVID-19.3
Types of Blood Oxygen Level Monitors
There are five types of SpO2 devices in everyday use. In rank order of best selling oximeters, they are the fingertip, handheld, smartphone apps, desktop, and wristbands. Wristbands are the newest devices on the market, with one model achieving FDA approval thus far. A brief description of each type is below.
Fingertip
The first and most used is the fingertip model. This type is compact, fits on the tip of a finger, and has the computer, light emitters, LED display, and photodetector all in one piece. They are highly portable and easy to use. They monitor at-risk patients for oxygen deprivation, patients using oxygen therapy, CPAP patients, athlete training, and homecare.4
Handheld
The handheld devices are larger than the small fingertip models but are still highly portable. There are usually 3-pieces to this model type—sensor, cable, and the LED screen with functional buttons. Often the sensor and cable combine to be a single piece to make the device a 2-piece unit. These SpO2 devices tend to offer slightly better readings and more functions. Handheld models are a favorite for clinicians because they are compact, easy to use and easy to store.5, 6
Desktop
Desktop models are a work-horse for hospital care. They are more extensive and often integrated with numerous monitoring functions. The LED screens are usually in color and large to display several different graphs to show histograms and trends. Numerical data on the screen indicate current readings. Several options are available that mount to an I.V. pole and others that are standalone units with wheels and an extension for bedside patient monitoring.7
Wristbands
Wristband models offer unintrusive continuous monitoring with an easy to read LED display. They provide comfort, reliability, and accuracy. The best wristbands work by embracing the ulnar wrist bone; thereby, some models do not require a fingertip probe. The Oxitone-1000 is currently the only model to achieve FDA approval.8
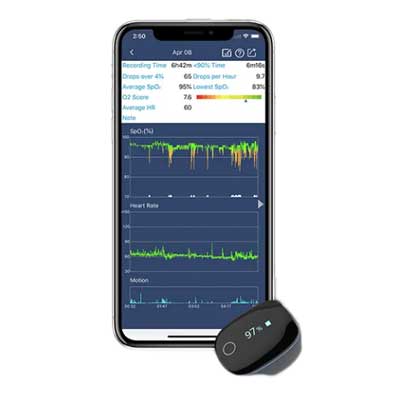
Smartphone Applications
Yes, there is an app for that! Smartphones can do almost anything these days, including monitoring patient oxygenation. Medical studies find these devices to be accurate and to offer some advantages over standard devices.9, 10 People can download an app from Apple or Google Play, purchase a sensor, and attach it to the smartphone, and they now have a personal SpO2 device. Many clinicians use the app on a tablet to take advantage of a larger screen for scanning patients.
Selecting the Best Pulse Ox
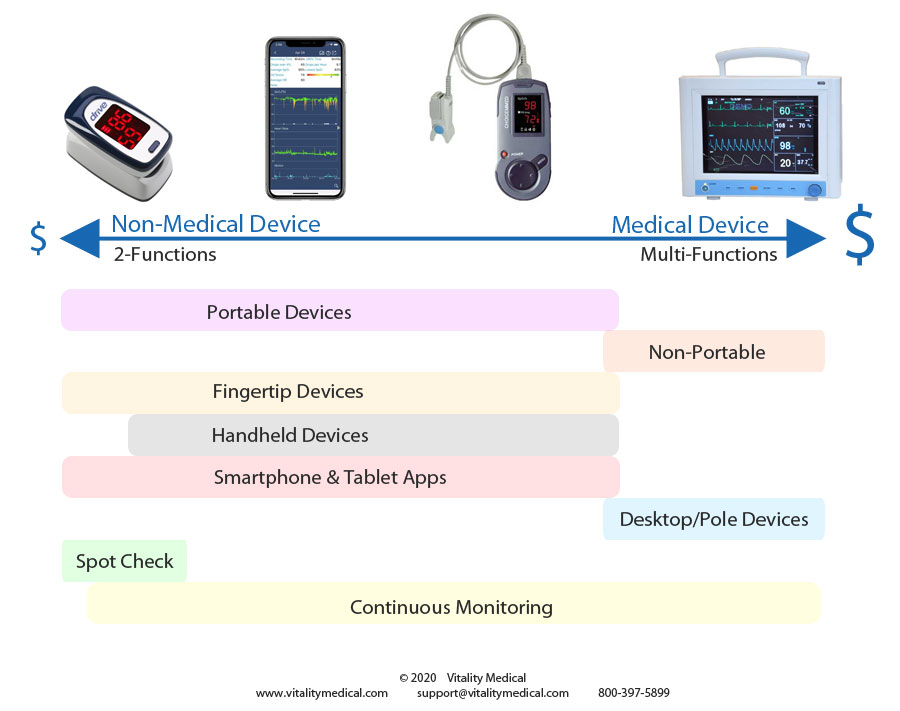
The continuum above portrays the different heart rate, and O2SAT devices and where they lie on a continuum of oxygen diagnostic monitors. Devices on the left of the continuum tend to be lower priced and have fewer functions, while those to the right cost more and have multiple functions. Very few of the fingertip devices provide more than the O2SAT standard functions of heart rate and blood oxygen saturation level.
Most of the SPO2 testers, particularly for homecare use, are fingertip or handheld devices. The larger desktop models and those attached to an I.V. pole offer multi-functions and larger displays with graphs. The desktop and pole models also offer continuous monitoring. A significant number of fingertips and handheld devices only offer spot-checking. Some new portable devices offer workout-tracking but determining the fakes from a bonafide SPO2 tracker may be difficult. Some manufacturers are touting watches that can provide continuous SaO2 tracking for physical workouts. Still, most are suspect because of the requirement to transmit two types of light waves and receive those waves in a photodetector. Unless the manufacturer can integrate a quality photodetector into the watchband, it is highly unlikely that a watch will provide accurate SaO2 readings except for the Oxitone-1000.
FAQ's
Are oximetry devices accurate?
Yes, most of these devices will give an accurate reading within 2%. Patients with cold hands, poor circulation, or nail polish may provide less accurate readings.
Which SaO2 device is the most accurate?
The most accurate measures for oxygenated blood is from an arterial blood gas test measured directly from arterial blood. An artery in the arm furnishes the blood through a puncture in the skin to the artery. This direct method provides the most accurate reading for blood gases, including both oxygen and carbon dioxide. An O2 meter is an indirect and painless exam using light wavelengths to measure oxygen density.
What is hyperoxia?
Hyperoxia is a blood condition in which the blood cells are oxygen deficient.
What is Normoxia?
Normoxia is a normal oxygen blood saturation condition. Device readings between 95 to 97% oxygen density are normal.
What is a regular heart rate?
The standard resting heart rate is between 60 to 100 beats per minute. People in excellent physical condition often have a lower heart rate than others.
What are the two sets of numbers for on an O2SAT reader?
One number indicates the percentage of blood oxygen saturation. The ideal value for this indicator is 95 to 97%.
The second number indicates the number of beats per minute. This number should range from 60 to 100.
Some devices may display other numbers that measure other essential factors, such as Pi, RRpTM, and PVi. Pi indicates the Perfusion Index that shows blood circulation strength. RRpTM displays the number of breaths per minute. This indicator helps to determine heart and lung functioning. PVi is the Pleth Variation Index, which monitors changes in hydration, breathing effort, and perfusion.
Vitality Medical carries O2 Sensor Probes, batteries, and other accessories for blood oxygen monitors. There is also a wide variety of Oxygen Supplies for Respiratory Therapy patients.
O2SAT Top Brands
Below is a list of the top-ranking brands of O2 Monitors. These manufacturers are highly respected and innovative in the medical supply industry.
Top Brands
1. ChoiceMMed
2. Innovo
3. Zacurate
4. Masimo
5. Drive Medical
6. Nonin
7. Medtronic Covidien
8. Medline PulSTAT
9. Hopkins Medical
10. Oximeter Plus
Footnotes
- Katella, Kathy. "Should You Really Have a Pulse Oximeter at Home?" Yale Medicine. May 8, 2020. (Last Accessed October 21, 2020)
- Pedersen T, Moller AM, Pedersen BD. Pulse oximetry for perioperative monitoring. systematic review of randomized, controlled trials. Anesthesia and Analgesia 2003; 96: 426-31. (Last Accessed October 21, 2020)
- Katella, 2020. (Last Accessed October 21, 2020)
- Carroll, Patricia. "Pulse oximetry-at your fingertips." RN 60.2 (1997): 22-27. (Last Accessed October 21, 2020)
- Heaton, Larry Christopher, et al. "Handheld four-wavelength retinal vessel oximeter." Ophthalmic Technologies X. Vol. 3908. International Society for Optics and Photonics, 2000. (Last Accessed October 21, 2020)
- Parameswaran, G. Iyer, Kathy Brand, and James Dolan. "Pulse oximetry as a potential screening tool for lower extremity arterial disease in asymptomatic patients with diabetes mellitus." Archives of internal medicine 165.4 (2005): 442-446. (Last Accessed October 21, 2020)
- Harris, Bronwyn U., et al. "Accuracy of pulse oximeters intended for hypoxemic pediatric patients." Pediatric Critical Care Medicine 17.4 (2016): 315-320. (Last Accessed October 21, 2020)
- Guber, Alexander, et al. "Wrist-Sensor Pulse Oximeter Enables Prolonged Patient Monitoring in Chronic Lung Diseases." Journal of medical systems 43.7 (2019): 230. (Last Accessed October 21, 2020)
- Chan, C., et al. "A smartphone oximeter with a fingertip probe for use during exercise training: usability, validity and reliability in individuals with chronic lung disease and healthy controls." Physiotherapy 105.3 (2019): 297-306. (Last Accessed October 21, 2020)
- Craven, Michael P., et al. "User requirements for the development of smartphone self-reporting applications in healthcare." International Conference on Human-Computer Interaction. Springer, Berlin, Heidelberg, 2013. (Last Accessed October 21, 2020)
Medical Studies























Login and Registration Form